Does Tattoo Ink Cause Cancer?
Nearly one in three adults has at least one tattoo. With that level of mainstream adoption, the question of long-term health consequences is legitimate—and increasingly studied. No confirmed cancer case has been directly attributed to tattooing, but a growing body of research suggests the relationship between tattoo ink and cancer is more nuanced than a simple yes or no. Here’s what the science actually shows.
What’s Actually Inside Tattoo Ink?
Most people assume tattoo ink is a purpose-built, medically reviewed substance. It isn’t. There is no ink formulated exclusively for tattooing—the pigments used in popular tattoo ink brands are the same pigments found in paints and textile dyes. This matters because industrial pigments were never designed to be injected into human skin.
Tattoo ink is deposited into the dermis, the deeper layer of the skin beneath the surface epidermis. Once there, it stays—permanently. The particles are too large for the body’s immune cells to fully break down, which is exactly what creates the lasting visual effect. But permanence cuts both ways.
Analysis of tattoo inks by Australia’s National Industrial Chemicals Notification and Assessment Scheme (NICNAS) examined 49 different tattoo inks and found significant discrepancies between what was listed on labels and what was actually inside the products. The findings raised immediate concern.
Hazardous Substances Found in Tattoo Inks
| Substance | Found In | Health Classification |
|---|---|---|
| Polycyclic Aromatic Hydrocarbons (PAHs) | 83% of black inks tested; 20% of all samples | Known carcinogen (WHO/IARC) |
| Azo Pigments | Nearly all ink colors except black and red | Break down into carcinogenic aromatic amines under UV/bacteria |
| Barium | White inks | Hazardous heavy metal |
| Copper / Cobalt | Blue/green inks | Potentially toxic at accumulation |
| Mercury / Cadmium | Red inks (mercury largely replaced by cadmium) | Toxic heavy metals |
| Nickel / Chromium | Various colors | Allergens; nickel classified as carcinogen |
| Arsenic | Trace amounts in various inks | Known carcinogen (IARC Group 1) |
PAHs alone—found in the majority of black inks—are classified by the WHO’s International Agency for Research on Cancer as known carcinogens. These are the same chemicals associated with elevated cancer risk in firefighters and petroleum workers through occupational exposure.
How Tattoo Ink Moves Through Your Body
The assumption that tattoo ink stays where it’s placed is incorrect. Research has confirmed that ink particles migrate away from the tattoo site through the lymphatic system—the body’s filtration and immune network.
When ink enters the dermis, macrophages (immune cells) attempt to engulf and neutralize the foreign particles. For larger particles, this process is largely unsuccessful. The macrophages absorb what they can and transport those particles through lymphatic vessels toward the lymph nodes—small, bean-shaped organs distributed throughout the body that filter waste and coordinate immune responses.
Ink particles have been detected in lymph nodes within weeks of tattooing. Over years and decades, accumulation increases—particularly for individuals with large or multiple tattoos.
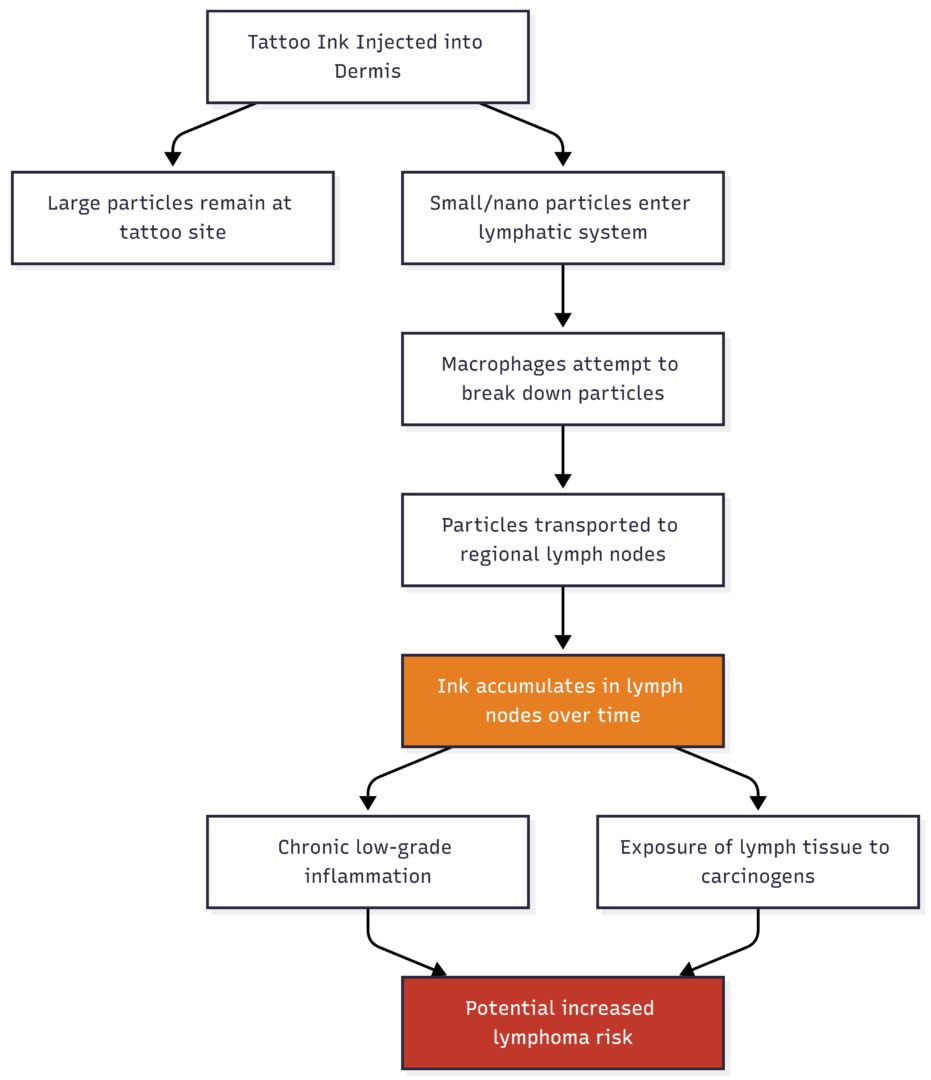
According to researchers at the University of Southern Denmark (SDU) and the University of Helsinki, this accumulation may cause the immune system to enter a state of sustained response—constantly recognizing ink as foreign matter and attempting to neutralize it. The concern is that this chronic immune activation could, over time, damage lymph node function or promote abnormal cell growth.
“We can see that ink particles accumulate in the lymph nodes, and we suspect that the body perceives them as foreign substances,” explained Henrik Frederiksen, consultant in haematology at Odense University Hospital. “This may mean that the immune system is constantly trying to respond to the ink, and we do not yet know whether this persistent strain could weaken the function of the lymph nodes or have other health consequences.”
What Does the Research Say About Lymphoma?
Lymphoma is a cancer originating in the lymphatic system, with roughly 90,000 newly diagnosed cases annually in the US. Known risk factors include age, certain viral infections, chemical exposure (notably benzene and pesticides), family history, and immune disorders. Tattoos are not an established risk factor—but researchers are investigating whether they should be.
A large European study comparing over 1,300 lymphoma patients with more than 4,000 controls without lymphoma found that lymphoma was 21% more common among tattooed individuals. However, the timing of tattoo exposure showed a non-linear pattern:
| Time Since Tattooing | Observed Lymphoma Risk Change | Statistical Significance |
|---|---|---|
| Within 2 years | +81% higher risk | Notable; may reflect immune activation |
| 3 to 10 years | No definite increase detected | Inconclusive |
| 11+ years | +19% higher risk | Modest; possibly reflects long-term accumulation |
Importantly, nearly all individual differences between groups failed to reach statistical significance. The study also found no correlation between the number or size of tattoos and lymphoma risk—which, if the ink were a direct cause, would be expected to show a dose-response relationship.
A separate Danish study using twin pair data—where one sibling was tattooed and one was not, sharing the same genetics and childhood environment—found a stronger signal. Among individuals with large tattoos (defined as larger than the palm of a hand), lymphoma rates were nearly three times higher than among non-tattooed counterparts. The Danish Twin Tattoo Cohort included data from more than 5,900 twins, providing a level of genetic control rarely available in observational research.
Jacob von Bornemann Hjelmborg, professor of biostatistics at SDU, explained the advantage: “We can compare twin pairs where one has cancer, but they otherwise share many genetic and environmental factors. This provides us with a stronger method for investigating whether tattoos themselves may influence cancer risk.”
Tattoos and Skin Cancer: A Separate Question
The relationship between tattoos and skin cancer involves different mechanisms than lymphoma and warrants separate consideration.
One population-based study found that tattooed individuals had a 29% higher risk of developing melanoma compared to those without tattoos, even after controlling for UV exposure, tanning bed use, and skin type. Among melanoma cases reviewed, 22% of patients had been tattooed before diagnosis versus 20% of controls—a small gap that nevertheless persisted after statistical adjustment.
Significantly, only 30% of melanoma cases in this study occurred at the actual tattoo site. This rules out a simple direct-damage explanation and points toward something systemic—likely the same immune and chemical pathway implicated in lymphoma risk.
There is an additional, practical concern: tattoos can physically obscure moles. Dermatologists use mole changes as a primary early indicator of melanoma. A tattoo placed over or near a mole removes that surveillance option. Ink pigmentation in the skin can also interfere with clinical assessment, delaying diagnosis.
On the other side of the data: a separate study found that individuals with three or more large tattoos had a 74% lower risk of melanoma compared to non-tattooed individuals. This counterintuitive result is unexplained and illustrates the current state of the evidence—inconsistent enough that firm conclusions remain premature.
Ink Particle Size and the Laser Removal Problem
Two specific risk factors beyond ink composition deserve attention: particle size and tattoo removal.
Particle Size
Tattoo ink particles are intentionally manufactured at a size the body cannot efficiently break down—this is the mechanism behind permanent tattooing. If all particles were small enough for immune clearance, tattoos would fade rapidly. However, manufacturing inconsistency means some batches contain abnormally small nano-particles. Particles small enough to pass through a cell’s membrane can enter the cell directly and damage DNA—the kind of cellular damage that, under the right conditions, can initiate cancer development.
Laser Removal
Laser tattoo removal works by fragmenting ink particles into smaller pieces that the body can then clear. The problem is that this fragmentation process—particularly with inks containing azo pigments—can generate breakdown products including carcinogenic aromatic amines. These are the same nitrogen-based compounds released when azo dyes are exposed to UV light or certain bacteria. Research suggests lymphoma risk increases meaningfully during and after laser removal compared to simply having the tattoo.

Relative Risk vs. Absolute Risk: Understanding the Numbers
A “3.91 times higher risk” headline sounds alarming. Context matters.
Relative risk describes how much more likely an outcome is in one group versus another. Absolute risk describes the actual probability of the outcome occurring. If the baseline risk of developing skin cancer is 1%, a 3.91× relative risk means the tattooed individual’s risk rises to approximately 4%—still very low in absolute terms.
| Scenario | Baseline Risk (Hypothetical) | Relative Risk Increase | Absolute Risk After Tattoo |
|---|---|---|---|
| Skin cancer (large tattoo) | 1% | 3.91× | ~4% |
| Lymphoma (tattooed vs. non-tattooed) | ~0.5% | 1.21× | ~0.6% |
| Melanoma (tattooed) | ~2% | 1.29× | ~2.6% |
Elevated UV exposure—from sunbathing without protection or regular tanning bed use—carries a substantially higher absolute melanoma risk than current tattoo research suggests. The numbers, while worth monitoring, should not be interpreted in isolation from the broader cancer risk landscape.
The Confounding Problem: Correlation vs. Causation
The studies above cannot prove that tattoos cause cancer. They show association. This distinction matters enormously.
People who get tattoos may differ systematically from those who don’t in ways that are difficult to fully account for in study design. Research has shown that younger tattooed individuals are statistically more likely to engage in behaviors—tobacco use, alcohol consumption, sun exposure without protection—that independently increase cancer risk. While the twin study methodology controls for genetics and shared environment, it does not eliminate lifestyle divergence between siblings in adulthood.
Furthermore, if tattoo ink were a direct and significant lymphoma trigger, the dramatic increase in tattoo prevalence over the past two decades would be expected to produce a corresponding rise in lymphoma rates. That rise has not been observed in population data.
“Studying this link is challenging because cancer can take years to develop,” acknowledged the SDU research team. “This means that exposure in youth may not lead to illness until decades later, making it difficult to measure a direct effect.”
Regulatory Landscape and Ink Safety Standards
Tattoo ink has historically operated in a regulatory gray zone. The pigments used are industrial, not pharmaceutical, and in many countries are subject to minimal pre-market safety review.
The European Union implemented restrictions on thousands of chemicals permitted in tattoo inks, specifically targeting azo compounds and other substances with known toxicity profiles. Market audits following these regulations found products with toxic ingredients above permitted thresholds and banned pigments mislabeled as compliant alternatives—indicating enforcement challenges.
The European standard ResAP(2008)1 sets out safety requirements and criteria for tattoo inks, and asking your tattoo artist whether their inks comply with this standard is a practical harm-reduction step.
In the US, the FDA has not issued equivalent restrictions at the time of writing. However, growing research attention and industry pressure have led some ink manufacturers to voluntarily reformulate products using safer pigment alternatives and improve labeling accuracy. These reformulated inks tend to cost more, which may gradually translate into higher tattoo pricing.
Practical Risk Reduction for People With or Considering Tattoos
- Choose a licensed, reputable tattoo artist who uses inks from established manufacturers with transparent ingredient labeling.
- Ask whether inks comply with ResAP(2008)1 or equivalent safety standards.
- Never tattoo over or adjacent to moles without prior dermatological clearance.
- Maintain regular skin checks—self-examination and annual dermatologist visits—regardless of tattoo status.
- Be cautious with laser removal: discuss the specific inks used in your tattoos with a qualified laser specialist, as removal of azo-pigment inks carries distinct risk considerations.
- Report any new or changing skin features in or around tattooed areas to a dermatologist promptly.
What Researchers Are Investigating Next
Current gaps in the evidence are well recognized by the researchers themselves. The next phase of investigation includes:
- Molecular-level analysis of how ink particles affect lymph node function over time
- Identification of which specific lymphoma subtypes show the strongest association with tattoo exposure
- Dose-response studies examining whether total ink volume (tattoo coverage area) correlates with cancer risk in a linear fashion
- Long-term cohort studies capable of tracking tattooed individuals from early adulthood through the latency period when cancers typically emerge
The Danish Twin Tattoo Cohort, with its genetically controlled methodology, will likely continue producing some of the most informative data as follow-up periods lengthen.
The Bottom Line
No study has proven that tattoos cause cancer. What the evidence shows is a statistical association—modest in most studies, more pronounced in others—between tattoo exposure and elevated rates of lymphoma and certain skin cancers. The biological mechanism is plausible: ink particles containing known carcinogens migrate to lymph nodes, accumulate over decades, and may trigger the kind of chronic immune activation linked to abnormal cell growth.
The absolute risk increase remains small. UV exposure, smoking, and alcohol use carry far larger cancer risk burdens. But the association exists, the chemistry supports concern, and regulation of tattoo ink composition has lagged far behind the industry’s growth.
For anyone with existing tattoos, the practical guidance is unchanged from general preventive health: regular skin checks, dermatologist access, and awareness of changes in tattooed or adjacent skin. For anyone considering a tattoo, understanding what’s in the ink—and choosing artists who prioritize regulated, transparent products—is the most actionable form of risk reduction currently available.
Please share this Does Tattoo Ink Cause Cancer? with your friends and do a comment below about your feedback.
We will meet you on next article.
Until you can read, Michelle Williams and the Art of the Butterfly Tattoo